
January 24, 2022
Today, people suspected of having inflammatory bowel disease are often required to undergo a colonoscopy, an invasive procedure performed under anaesthesia. A new method developed at the Weizmann Institute of Science in collaboration with the Sheba Medical Center at Tel Hashomer may offer a non-invasive alternative: detecting inflammation in the intestines by analysing a faecal sample.
In future, stool testing might facilitate the diagnosis of disorders such as Crohn’s disease and ulcerative colitis and help monitor their course, as well as enable physicians to select the most appropriate therapy for each patient. The study’s findings are being published this week in the journal Gut.
The idea for this study was born when researchers in the lab of Professor Shalev Itzkovitz of Weizmann’s Molecular Cell Biology Department saw that cells shed from the gut lining of mice and expelled in the faeces stay alive for several hours.
“We realised that we could analyse gene expression in cells shed daily from the lining of the human gut, using this expression to learn about potential disease processes in the intestines,” said Itzkovitz, who headed the research team.
Dr Bella Ungar, a gastroenterologist at Sheba Medical Center, led the study, in which she and other researchers from Sheba and Weizmann analysed cells collected from the gut lining of thirty patients with inflammatory bowel disease during the course of colonoscopy.
Some of the cells came from faecal samples taken from the lower intestinal tract, others from biopsies of the gut lining in the same area. The researchers compared the cells collected from the patients with those taken from faecal samples or biopsies of some thirty healthy people who had undergone colonoscopies as part of routine cancer screening.
Using specially adapted RNA sequencing and other advanced methods, the scientists determined which cell types were present in each of the samples. They found that apart from the regular cells making up the gut lining, the faecal samples contained four immune-related cell types associated with inflammation, among them inflammatory monocytes and regulatory T cells.
By means of algorithms developed in Itzkovitz’s lab, they then identified distinct expression patterns, or RNA signatures, of the cells in each sample. These signatures helped reveal the exact proportion of each immune-related cell type in the gut lining; no less important, they enabled the scientists to determine whether or not a person had an active case of intestinal inflammation.
The faecal samples proved to be more reliable in this respect than the biopsies.
“A biopsy can miss inflammation because it provides a snapshot of the narrow spot from which it was removed, whereas a faecal sample contains cells shed from the entire lining of the gut,” Itzkovitz explained.
“Moreover, a faecal sample can sometimes be more revealing than the examination of the lining during colonoscopy, which is done by eye, because certain forms of inflammation produce no visible signs.”
Reading out the RNA signatures of cells from faecal samples can be crucial for selecting a personalized therapy – for example, administering drugs designed to block only the types of substances triggering inflammation in a particular patient, rather than suppressing that person’s entire immune system. Such therapies already exist – new biological drugs that bring dramatic relief to some patients with inflammatory bowel disease – but it’s currently impossible to know in advance which drug will help which patient.
Overall, these drugs still work in only about half of those who receive them. Knowing which subsets of inflammatory cells are responsible for the disease process and which genes they express could improve the effectiveness of therapies, giving physicians crucial information before they prescribe the drugs. In addition, having a quick and simple way of assessing intestinal inflammation may help determine when the therapy is needed and when it can be stopped.
Ungar points out that the faecal RNA signature method is different from medical tests developed in the past to check the stool for signs of intestinal inflammation; one of them, for example, measured the levels of a protein called calprotectin. Those tests were not highly reliable, and thus colonoscopy has remained the gold standard for evaluating inflammation in the intestines, even though it’s invasive and requires cumbersome preparation.
The new Weizmann-Sheba method could provide testing for inflammation that is less invasive, much cheaper than colonoscopy and at least as reliable.
Also participating in the study were Miri Yavzori, Dr Ella Fudim, Dr Orit Picard, Professor Uri Kopylov, Professor Rami Eliakim, Dr Chen Mayer, Professor Iris Barshak and Professor Shomron Ben-Horin of the Sheba Medical Center; Dr Dror S. Shouval of Schneider Children’s Medical Center of Israel; Dr Yishai Levin and Dr Alon Savidor of the Nancy and Stephen Grand Israel National Center for Personalized Medicine; and Dr Shani Ben-Moshe, Dr Rita Manco, Stav Dan, Adi Egozi and Dr Keren Bahar Halpern of Weizmann’s Molecular Cell Biology Department.

(l-r) Dr Bella Ungar and Professor Shalev Itzkovitz. Cooperation between scientists and physicians
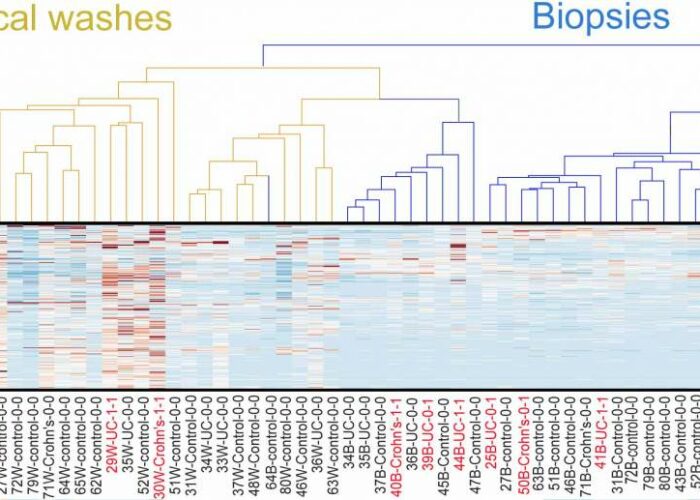
Expression of inflammatory genes (reddish-brown) in intestinal cells is evident in fecal samples (left) but not in samples obtained by biopsy (right)






