
October 16, 2021
Immunotherapy has sparked new hope for people with cancer, but for it to work, the patient’s immune system must be able to ‘see’ the tumour. There are ways of enhancing this recognition in individual cases, yet such solutions are, by definition, personalised, which greatly limits their use.
Professor Yardena Samuels and her PhD student Dr Aviyah Peri at the Weizmann Institute of Science, together with their colleagues, have now developed a method for identifying cancer ‘hotspots’, features that are common to many tumours and can therefore be used to develop effective immunotherapy for entire groups of patients.
The researchers have already used the method to identify a hotspot characteristic of a particularly aggressive form of melanoma in one major subset of patients. The study was just published in the Journal of Clinical Investigation.
Cancer hotspots are physical structures on cancer cells’ outer membranes that can provide the immune systems of multiple patients with ‘access’ to a tumour. These molecular structures contain mutated peptides called neoantigens that the immune system’s T cells recognize as foreign – the first step in binding to the neoantigens and killing the cancerous cells. In fact, this T cell action is the ultimate goal of all types of immunotherapy, so scientists have been using neoantigens to prime T cells for a successful attack.
However, since most neoantigens result from unique mutations characteristic of individual tumours, when a particular neoantigen is used to activate a patient’s T cells, the same therapy cannot be applied to other patients. Only a handful of neoantigens – those derived from recurrent mutations appearing in numerous patients – qualify as hotspots, but these are hard to find. Part of the difficulty stems from the fact that the neoantigens on the cellular membranes are presented to the immune system by protein complexes called HLA, and these complexes come in thousands of versions, so together with the cancerous mutations, there can be millions of individual variations.
Because of this enormous variability, hotspot neoantigens have until now been found mostly by luck. In the new study, a team headed by Samuels, of Weizmann’s Molecular Cell Biology Department, has developed a method for identifying these cancer hotspots in a systematic manner. Referred to as a “data-driven approach to identifying recurrent neoantigens,” it involves bioinformatics followed by lab analysis.
Peri led the study, conducted in the Samuels lab with the late Professor Nir Friedman of Weizmann’s Immunology Department, Professor Masha Y. Niv of the Hebrew University of Jerusalem, Professor Steven A. Rosenberg of the National Cancer Institute, USA, Professor Cyrille J. Cohen of Bar-Ilan University, Dr Ansuman T. Satpathy of Stanford University School of Medicine and other researchers.
As the first step, the scientists applied algorithms to search through international databases containing information on the genomes of thousands of cancer patients. Focusing on melanoma, the main cancer type studied by the Samuels lab, they surveyed oncogenes, looking for common mutations presented by common forms of HLA. The team’s search produced a number of neoantigens that could potentially be considered hotspots. Next, the scientists subjected these candidate molecules to laboratory analysis known as HLA peptidomics, in which they isolated the mutant peptides from the HLA complexes and investigated their interactions with T cells.
Using this approach, the scientists identified a hotspot neoantigen derived from an oncogene known as RAS, which is involved in causing a third of all human cancers. This neoantigen, belonging to a form of RAS that causes a particularly aggressive form of melanoma, appears in some 20 percent of melanoma cases. In collaboration with Friedman and Satpathy, the scientists isolated the T cell receptor that can recognize this hotspot neoantigen in melanoma tumors. They then engineered T cells from healthy individuals to express this receptor and incubated them in a test tube with tumor samples from patients whose tumors displayed this hotspot. The T cells were activated by the neoantigen, killing the tumor cells in a highly specific manner – that is, only those cells that displayed the neoantigen.
“We’ve uncovered a neoantigen that is expressed in thousands of new melanoma cases every year, and we’ve shown that it can be used in these patients to mark tumor cells for immune destruction,” Peri says.
“Our study suggests that our newly developed platform can lead to ‘off-the-shelf’ immunotherapies in which T cell receptors that recognise cancer hotspots can be prepared in advance, ready to be applied in groups of patients whose tumors have been shown to harbor these hotspots,” said Samuels.
Such treatments would be easier and cheaper than tailoring personalized T cells to each new patient.
Yet another major advantage of this approach is that it makes use of hotspot neoantigens derived from oncogenes. When an oncogene like RAS is active in a tumor, it is expressed in all tumor cells. This means that the hotspot immunotherapy is more likely to wipe out the entire tumor, rather than only parts of it, as was the case with therapies that targeted neoantigens present in only some of the tumour cells.
“Our novel approach may make it possible to apply personalized treatments on a larger scale than today,” Samuels said.
“It is ready to be developed for use in hospitals, and it can be applied to a variety of cancers, not only melanoma.”
Yeda Research and Development Company, the Weizmann Institute’s technology transfer arm, is currently seeking to promote the method’s development for clinical use, through a company that is being established to this end.
Study participants also included Erez Greenstein and Dr Shlomit Reich-Zeliger of Weizmann’s Immunology Department; Dr Michal Alon, Dr Shelly Kalaora, Chaya Barbolin, Dr Ronen Levy and Polina Greenberg of Weizmann’s Molecular Cell Biology Department; Joy A. Pai of Stanford University School of Medicine; Dr Tamir Dingjan of the Hebrew University of Jerusalem; Dr Eilon Barnea and Professor Arie Admon of the Technion – Israel Institute of Technology; Claudia Arnedo-Pac and Prof. Nuria Lopez-Bigas of the Barcelona Institute of Science and Technology; Dr Bareket Dassa and Dr Ester Feldmesser of Weizmann’s Life Sciences Core Facilities Department; Ping Shang, Dr James S. Wilmott and Professor Richard A. Scolyer of the University of Sydney; Dr Yishai Levin of the Nancy and Stephen Grand Israel National Center for Personalized Medicine; Dr Gil Benedek and Professor Michal Lotem of the Hadassah University Medical Center; Professor Mitchell P. Levesque of the University of Zurich; Professor David J. Adams of the Wellcome Sanger Institute; and Dr Goran B. Jonsson of Lund University.
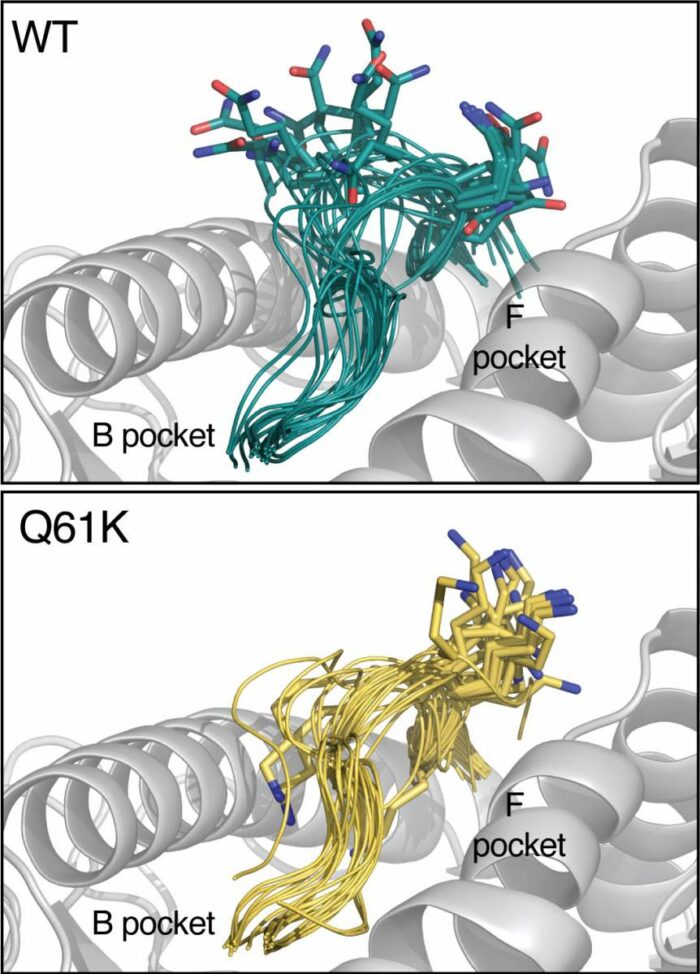
HLA complex (grey) expressed by skin cells. Bottom: “hotspot” identified by the team of researchers (yellow); Top: wild-type peptide without mutation (turquoise)

Professor Yardena Samuels. Identifying cancer "hotspots"





